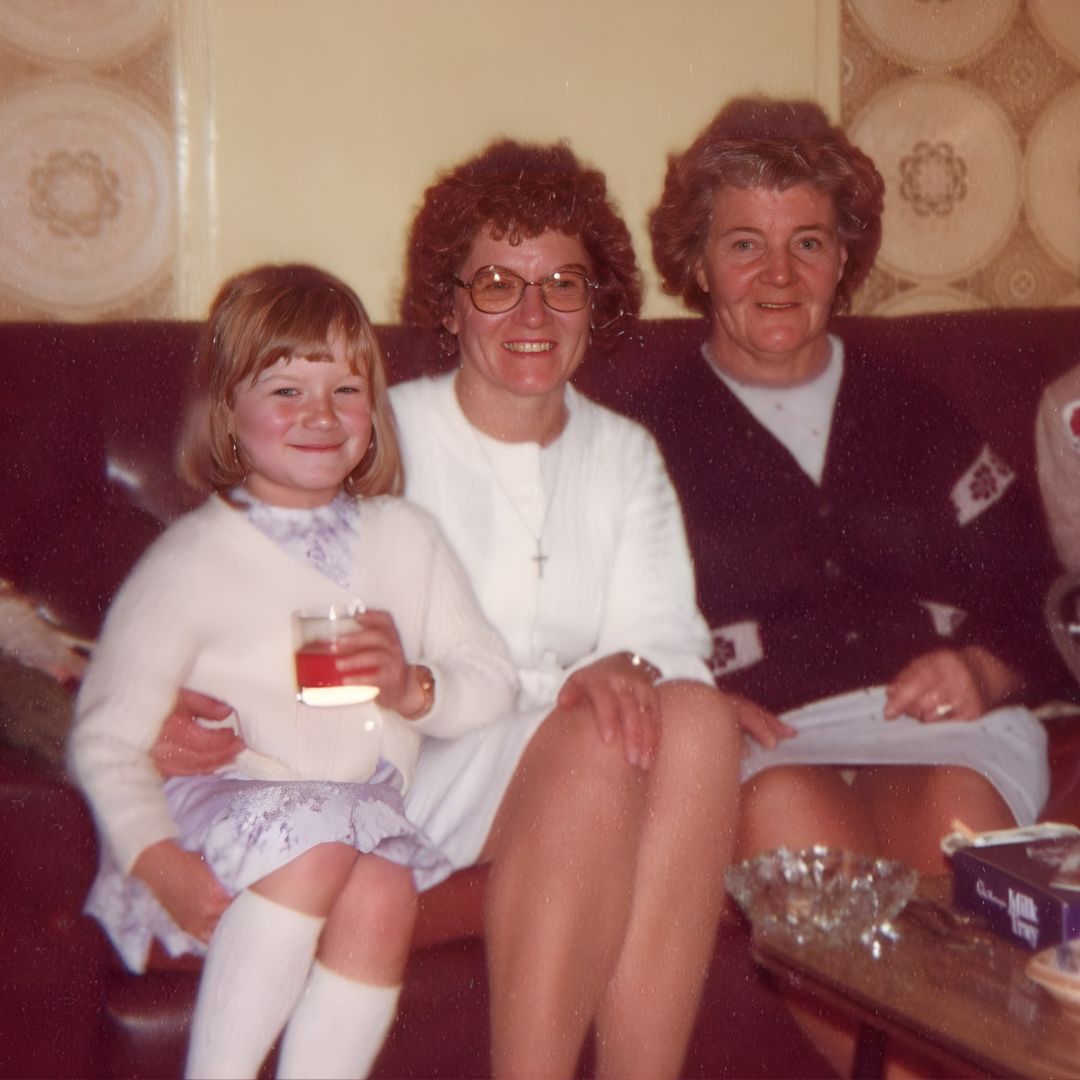The Trip That Started a Conversation
It was the summer of 1989. I was 17, two years into a Crohn’s disease diagnosis, and our family had been on a trip to France. We missed the ferry home and found ourselves stuck — in an unfamiliar place, no toilet in sight.
I was in the middle of a flare-up. Every journey away from home carried its own anxiety back then — the constant calculation of where the nearest toilet was, how long I had, whether I’d make it in time. But Crohn’s was never going to stop me living, a decision I made soon after diagnosis, and that was why I was panicking and desperately running around France in search of a toilet.
We found somewhere – eventually. I got inside the cubicle. However, it still wasn’t enough.
If you’ve lived with Crohn’s, colitis, or severe IBS, you’ll know exactly what that means. I was devastated and humiliated in a way that stays with you, especially at age 17.
But something unexpected came out of that moment. My Nanna opened up to me.
She’d been struggling with constipation for years — quietly, the way people did. Nobody talked about gut problems then. But watching me deal openly with what my body was doing gave her permission to speak. For the first time, she felt she could say it out loud. Because I understood, and was living it every day.
We don’t talk about our gut. And that silence costs people more than embarrassment.
That dynamic is still at the heart of what I do. My clients tell me things they’ve never said to their GP — about urgency, accidents, symptoms they’ve quietly reorganised their lives around. The conversation has to start somewhere.
For my Nanna, it started on that trip. But it didn’t go far enough.

We don’t talk about our gut.
And that silence costs people more than embarrassment.
Questions My Nanna Never Got to Ask
Within about a year of that conversation, my Nanna was admitted to the hospital as an emergency. They operated, removed a growth from her bowel, and sent it for biopsy.
Then she was sent home. No follow-up treatment or monitoring. Nobody saying: we need to keep watching this.
She trusted that if something needed doing, someone would tell her what she needed to know. She didn’t know what questions to ask — and nobody offered the answers.
Within another year she was diagnosed with bowel cancer. Given four years to live. She died within eleven months, in her mid-sixties, not long after retiring.
My great-grandmother — her mother — had also died of bowel cancer. A thread nobody had connected and one I only learned of fairly recently.
I live with Crohn’s disease, and that family history puts me at significantly higher risk of bowel cancer. Because of it, regular surveillance colonoscopies are part of my life. Knowing my risk matters — and so does advocating for it. Most people don’t know they need to do the same.
What Happens When We Add External Rhythm
The human nervous system has a natural tendency toward entrainment — the process by which biological rhythms synchronise with external cues.
You See This In Music.
You See It In Movement.
You even see it in how people unconsciously match pace when walking together.
Research in rhythmic auditory stimulation shows that steady external beats can influence neural timing, attention, and autonomic regulation.
When breathing is guided by a consistent rhythm — rather than internal counting — the body has something stable to synchronise with.
Instead of “trying to breathe correctly,” you begin to follow.
That shift alone reduces cognitive load.
And reduced cognitive load supports regulation.
A growth was found. A biopsy was done. She was sent home without follow-up.
That is how things get missed.
Gut Symptoms To Take Seriously
These are the gut symptoms to take seriously – and the reasons they so often get dismissed are that they overlap with IBS and common conditions. If you’re experiencing any of the following persistently, in combination, or as a change from your normal, speak to your GP:
- A persistent change in bowel habits lasting more than a few weeks
- Blood in your stool — bright red or darker
- Unexplained weight loss
- Persistent abdominal pain or bloating that doesn’t respond to what usually helps
- A feeling of incomplete emptying after going
- Unexplained fatigue, especially alongside other symptoms
Most of the time, these won’t be cancer. But they deserve investigation — not just management.
If something has changed and it’s not resolving — push for answers. You are allowed to ask more than once.
My Nanna didn’t know what questions to ask.
You do now.
Who Is at Higher Risk?
Bowel cancer is the UK’s second biggest cancer killer. Risk increases with age, but rates are rising in younger adults too. Higher risk factors include:
- Family history of bowel cancer in a first-degree relative
- A personal diagnosis of Crohn’s disease or ulcerative colitis
- A history of bowel polyps
- Lifestyle factors — low fibre, high processed meat, smoking, low activity
If any of these apply, mention it to your GP and ask specifically about your screening options. Don’t wait to be invited.
NHS Bowel Cancer Screening
Everyone in England aged 50 to 74 is sent a FIT test kit every two years — a simple home stool test that checks for traces of blood. If yours is sitting in a drawer, do it this week.
If you are aged 75 or over, you’ll need to call to request the test.
Under 50 with a family history or IBD diagnosis? Ask your GP whether earlier surveillance is appropriate for you.
Where My Work Fits In
Nutrition, nervous system regulation, and reducing chronic inflammation all support long-term bowel health — and many of the lifestyle risk factors for bowel cancer are things I work through with clients every day. That work sits alongside medical investigation and monitoring, not instead of it.
If a doctor has dismissed, minimised, or managed your symptoms without proper investigation — you are allowed to go back and ask again.

This April
See your GP if you have symptoms that have changed, persisted, or aren’t responding to what usually helps.
Do your FIT test if it’s waiting.
Tell your GP your family history and ask about your surveillance options if they apply.
And if you’d like support with your gut health alongside your medical care — book a free Gut Conversation.
Jungle-Trained. Science-Informed.

Nikkie Windsor UKIHCA-RHC
Integrated Nutritionist & Breath Coach
Gut issues stealing your freedom? I help mid-life adults get to the root of unpredictable digestion, stress-driven symptoms, and low energy — through nutrition, nervous system regulation, and breathwork.
I live with Crohn’s disease, so I know what it means to plan your life around your gut. And I know what it takes to stop.
Book a free Gut Conversation to explore your symptoms and map out your next steps.

Nikkie Windsor UKIHCA-RHC
Nutritionist, Health Coach & Breathwork Facilitator
Jungle-Trained. Science-Informed.
I help people navigating midlife move from gut chaos, low energy and overwhelm to steady digestion, resilient energy and confidence in their bodies again.
Book a personalised strategy call to explore your gut symptoms, energy and stress patterns — and map out your next steps.
Are You Ready to Change Your Gut Story?
You don’t have to manage this alone. Take the first step to feeling better today.